My Cpap Gave Me Life Again I Lost Weight I Wasnt Depressed
The people who finish breathing in their slumber
(Paradigm credit:
Getty Images
)

If you take sleep apnoea, chances are you don't realise it. But it's linked to diabetes, eye affliction and other conditions, and it can put your life at chance
I
I thought I was dying. During the twenty-four hour period, I was so tired my knees would buckle. Driving the car, my caput would dip and then I would catch myself. My face was lined with burnout.
At night, I would sleep fitfully, legs churning, then snap awake with a offset, gasping for breath, middle racing.
My doctor was puzzled. He ordered blood tests, urine tests, an electrocardiogram – maybe, he idea, the problem was eye affliction – those night-time palpitations…
No, my heart was fine. My blood was fine.
He ordered a colonoscopy. It was late 2008 and I was 47 years onetime – virtually time to be having one anyway. So I forced downward the iv litres (vii pints) of Nulytely to wash out my intestines so a gastroenterologist could take a skilful wait inside.
My colon was clean, the doctor told me when I regained consciousness. No cancer. Not even whatsoever worrisome polyps.
However, there was one thing.
"While yous were under," he said, "yous stopped animate at one point. You might want to check that out. It could exist sleep apnoea."
I had never heard of information technology.
You might also like:
- Why tin't some people think their dreams?
- The male child who stayed awake for 11 days
- The tragic fate of the people who end sleeping
Slumber is marked by dynamic changes throughout the body. It'southward made up of different phases, and every bit you move through them, your animate, claret pressure and body temperature will all autumn and rise. Tension in your muscles by and large stays the same as when yous are awake – except during REM phases, which account for upward to a quarter of your sleep. During these, most major musculus groups ease significantly. Simply if your throat muscles relax too much, your airway collapses and is blocked. The result is obstructive sleep apnoea – from the Greek ápnoia, or "breathless".
With slumber apnoea, your air supply is continually interrupted, causing blood oxygen levels to plummet. Yous then stir, gasping, trying to breathe. This tin can happen hundreds of times a night, and the ill-effects are many and severe.
Apnoea puts strain on the heart, as it races to pump blood more than apace to compensate for the lack of oxygen. Fluctuating oxygen levels also cause plaque to build up in the arteries, increasing the risk of cardiovascular affliction, hypertension and stroke. In the mid-1990s, the US National Commission on Sleep Disorders Inquiry estimated that 38,000 Americans were dying every year of heart disease worsened past apnoea.
In that location's also growing evidence that the condition affects glucose metabolism and promotes insulin resistance – leading to type 2 diabetes – and encourages weight proceeds.
Then at that place'due south the exhaustion of never having a full night's slumber, which is associated with memory loss, anxiety and low. Lack of sleep also causes inattention that can pb to traffic accidents. A 2022 report of drivers in Sweden plant that those with slumber apnoea are two.v times more likely to have an blow than those without. Information technology too fuels absenteeism, and people with apnoea are fired from their jobs more oft than those without.

Sleep apnoea means yous never get a good night's sleep, putting a strain on your body and mind (Credit: Getty Images)
One study found that people with severe sleep apnoea were, all told, three times every bit likely to die during an 18-yr period as those without.
Simply, as with smoking during the first decades later on it was discovered to be lethal, there'southward a disconnect between the harm that the status causes and the public's perception of it equally a threat. "They fail to link sleep apnoea with its many serious comorbidities," says a study deputed past the American Academy of Sleep Medicine, which estimates that information technology affects 12% of United states of america adults – but 80% go undiagnosed. This prevalence is as well found globally: nearly a billion people effectually the earth endure from mild-to-severe sleep apnoea, according to a 2022 report.
Research is now scrambling to take hold of upwardly. Medical science has been working overtime to find a solution, from in-depth studies of hypoxia – how the torso reacts to lack of oxygen – to new types of surgeries and appliances for treating the condition. Of the billion or so people across the earth struggling with slumber apnoea – most probably not even enlightened of it, never mind receiving treatment – I accept deep psychological insight into just 1: me. As the possibility that I could be facing an under-researched but potentially life-threatening wellness problem dawned on me, my central concern was simple: how tin I fix this?
While there are enduring risk factors for slumber apnoea – such as obesity, a large cervix or big tonsils, a small jaw, or getting older – it doesn't present itself until after an individual falls asleep. The but manner to diagnose it is to monitor someone's sleep.
And so in early on 2009, prompted past both exhaustion and the suggestion from my doctor, I made an appointment at a place called Northshore Sleep Medicine in Northbrook, Illinois.
I was met by Lisa Shives, a specialist in slumber medicine. She peered down my throat, and then suggested I take a polysomnogram – a sleep study, where my breathing, blood oxygen levels, heart rate, and encephalon and muscle activity would be recorded.
I returned for this a few weeks later, on a Thursday at 9pm.
A technician showed me into a small-scale sleeping accommodation containing a double bed and an armoire. Behind the bed, a horizontal window looked into a lab-similar room stuffed with equipment. I changed into some flannel sleep pants and called the technician back in. She stuck electrodes over my chest and head, then gave me a fishnet shirt to put on to concur the wires in place.
At nearly 10pm I clicked off the low-cal and presently fell comatose.
I woke up at 4.30am and fuzzily volunteered to endeavour to go back to sleep, simply the technician said they had half dozen hours of data and I was gratis to go. Subsequently I got dressed she told me that my apnoea was "severe" and that Shives would give me the details later on. I had planned to take myself out to a celebratory breakfast, but instead I but went domicile. I wasn't hungry – I was scared.
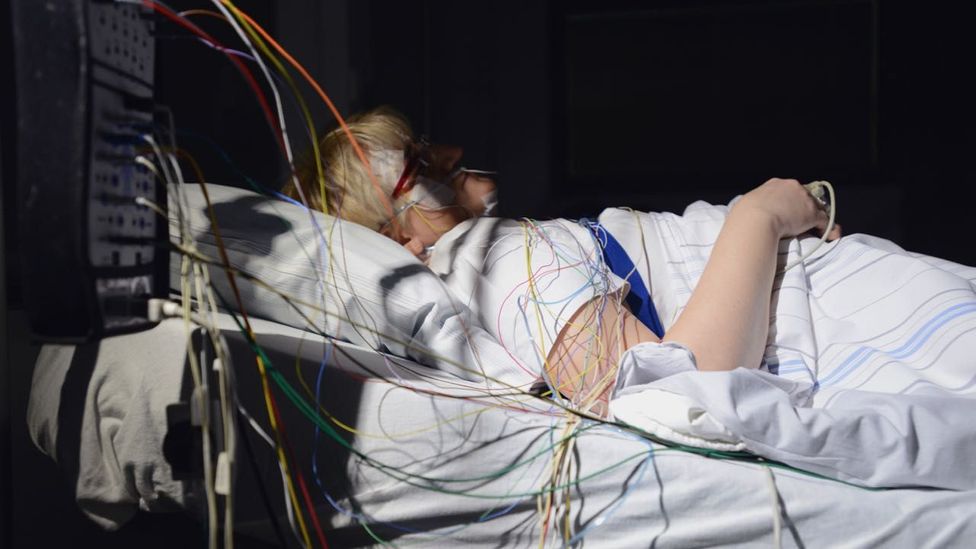
The only way to diagnose sleep apnoea is to monitor someone's sleep (Credit: Getty Images)
Several weeks later I was dorsum at Northshore, this time during daylight. Shives saturday me downwards in front of a screen full of multi-coloured squiggles and numbers, with a small black-and-white video of me sleeping in the corner. Information technology was unsettling, like seeing a crime scene paradigm of myself, dead.
Speaking of death, I had stopped breathing, Shives told me, for as long every bit 112 seconds – about ii minutes.
A normal level of blood oxygen saturation, as measured by a pulse oximeter, is between 95% and 100%. People with chronic obstructive pulmonary disease might accept a reading in the upper 80s. Mine at times had dipped to 69%.
How bad is that? The Earth Health System, in a surgical guide, suggests that should a patient'due south blood oxygenation fall to 94% or below, they should immediately be checked to encounter whether an airway is blocked, a lung has collapsed or there is a problem with their circulation.
My options were few. I could, Shives said, have a uvulopalatopharyngoplasty, a procedure as ghastly as its name: removing tissue from my soft palate and widening my airway at the dorsum of my throat. But it would be bloody, and recovery could be long and troublesome. Shives raised the possibility only to immediately dismiss it, which I afterwards suspected was to take the sting off the second option: the mask.
For the outset decade and a half after sleep apnoea was identified, there was simply one handling option. You could have a tracheotomy – a surgical process where a pigsty chosen a tracheostomy is cutting depression in your throat to featherbed your collapsing upper airway. It offered reliable relief but had pregnant complications of its own.
"In the early on days, doctors didn't know much," says Alan Schwartz, who recently retired as a professor of medicine at Johns Hopkins University in Baltimore after years of pioneering exploration on sleep ailments. "In the '80s, when I began, we were seeing the tip of the iceberg, the most severe apnoea patients. They'd wake upwards with a headache, from their bodies' tissues not getting enough oxygen. Feeling very fatigued, equally you might await. They'd get depressed, at that place were mood changes, short temper."

A 2022 study constitute that sleep apnoea might exist present in up to 40% of the general population in Germany (Credit: Getty Images)
Despite these woes, patients were understandably wary of having a tracheotomy, which today is "a surgical option of last resort" performed just in cases of extreme medical urgency.
"I was always a very loud, aggressive snorer, waking upward in the middle of the dark, gasping," says Angela Cackler of Hot Springs, Arkansas, who was diagnosed with sleep apnoea in 2008, though she believes it began when she was "tiny".
By 2012 her heart was failing.
"I went into the emergency room because I was really tired, non feeling well," Angela says. "I institute out it was centre failure. The side by side morning, they said, 'We are going to practise a tracheotomy.'"
And how has she adjusted to the tracheostomy after 7 years?
"Information technology'south a battle to deal with," she says. "There is a lot of cleaning. It'due south nasty. It'due south work. Y'all don't breathe usually. Your natural humidifier is completely gone. You have to supplement that. You're susceptible to infections." The biggest drawback for her is that information technology keeps her from swimming, a recreation she once enjoyed. She also hates the looks she gets from people.
That said, the procedure did eliminate her apnoea. "I don't snore and I can exhale and sleep amend."
Would she have information technology done once more?
"If I had to practise it again, aye, absolutely," she says. "It has saved me."
Though they piece of work in treating slumber apnoea, the life-altering drawbacks of tracheotomies inspired Colin Sullivan, today a professor of medicine at the University of Sydney, to invent the Continuous Positive Airway Pressure machine, or CPAP, that would go the new start-line treatment.
In the late 1970s, he had gone to the University of Toronto to help a slumber researcher investigate respiratory command in dogs during sleep. The research involved delivering experimental gases to dogs through a tracheostomy. Returning to Australia, Sullivan designed a mask that could fit around a domestic dog'due south snout to deliver the gases that way instead.
A human patient scheduled for a tracheotomy simply "eager to know if at that place was anything else that might piece of work" – Sullivan's words – inspired him to try to modify the dog mask for utilize by people.
Sullivan took plaster casts of patients' noses, creating a fibreglass mask that tubing could be attached to. The blower was salvaged from a vacuum cleaner, with a head harness crafted from the inside of a bicycle helmet.
In a 1981 paper, he and his colleagues described how, when fitting the mask over the noses of five patients, CPAP "completely prevented the upper airway occlusion".
Sullivan patented the device, and after a few years of development, he had a version that could be given to people with apnoea for use outside a lab. Today, millions use CPAP machines, though success oft requires perseverance.

CPAP machines are the start-line handling for sleep apnoea but many sufferers observe them frustrating to apply (Credit: Getty Images)
But as more than patients were treated and the CPAP machines' technology was refined – they tin now upload information automatically to the cloud for analysis – doctors made an unwelcome discovery: their primary treatment ofttimes didn't piece of work.
"In the tardily '80s, we'd sit downwards with a patient and ask, 'How's it going with the mask?'" recalls Schwartz. The patient would report, falsely, how well the mask was working. "Until we began to put electronic fries in the machines in the late '90s, nosotros never appreciated how footling they were using their machines."
The chips tracked how long the masks were used, and doctors found out they frequently weren't being worn at all. "The mask is like something from a bad science fiction motion-picture show: big, bulky and obtrusive," a New York Times article reported in 2012. Studies propose somewhere between a quarter and half of users abandon their machine within the start year.
I certainly did.
The CPAP did brand me feel better the first night I wore information technology – once more under ascertainment at Northshore. I woke refreshed, alert, feeling more than energised than I had in years.
But the positive effect of the mask tapered off considerably after that first deliciously restorative night. Outside of the lab I couldn't reproduce the benefits. That beginning C in CPAP is for continuous, significant that it pushes in air when y'all breathe in just it also pushes in air when yous exhale out. You are fighting against information technology equally you lot exhale, and I would wake up suffocating. There was the continual embrace of the mask, clamped to my confront. Air would leak out around the edges and dry my eyes, even though they were closed.
Almost nights at some point I would wake upwardly and rip the mask off. In the morning, I would check the stats and encounter how little it was working. I went back to Northshore, where Shives would fiddle with the force per unit area settings or encourage me to try other masks. I returned several times, and began to feel like a regular. Nothing seemed to work.
Finally Shives, exasperated, said, "You know, if you lost 30 pounds, the problem might become abroad."
While it is possible to be sparse and have sleep apnoea, obesity multiplies the probability.
I'm v'9 and weighed 150 pounds when I graduated from college. In 2009, I weighed 210 pounds.
So in 2010, I decided to lose the weight. I had a goal – the xxx-pound figure Shives recommended. And I did it, going from 208 pounds on 1 January 2010 to 178 pounds on 31 December. Losing the weight did the trick. No more than mask.
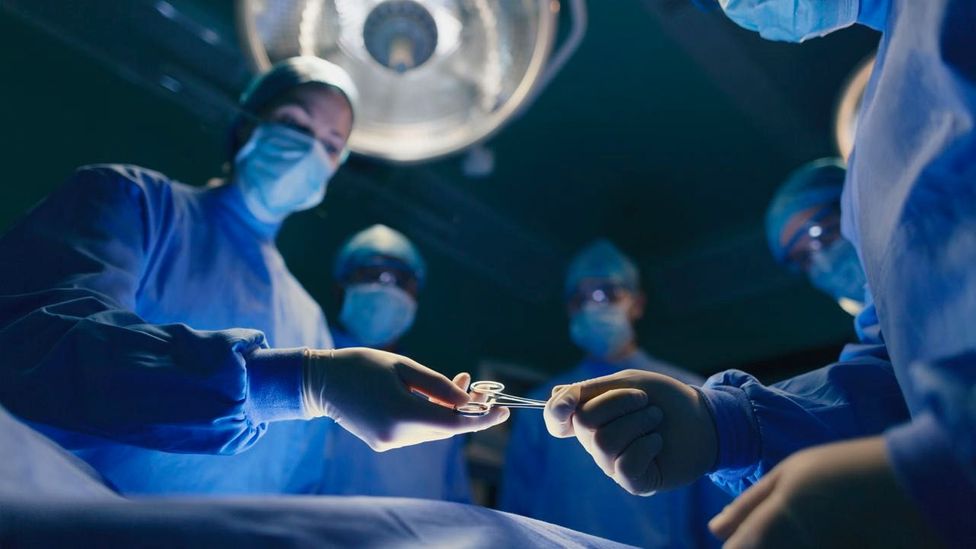
People with slumber apnoea are at increased risk for certain complications during surgery (Credit: Getty Images)
Only it turns out I mistook winning a single year'due south battle with victory in the war. The pounds I had lost somehow found me once again, 20 of the 30 creeping slowly back on over the next decade. And with them, the apnoea came dorsum. Non that I realised information technology until the summer of 2019, when I underwent spine surgery. The pre-surgery questionnaire at Northwestern Memorial Hospital in Chicago asked if I sometimes snored, if I was oftentimes tired and if I had ever been diagnosed with sleep apnoea.
Yes, yes and aye.
"It's of import to screen people for slumber apnoea considering information technology could be a risk when having surgery," says Phyllis Zee, managing director of the Center for Circadian and Sleep Medicine at Northwestern University'southward Feinberg School of Medicine. It tin be a chance factor for poor outcomes later too.
The questions nigh snoring and exhaustion are important because, despite the efforts of medical scientific discipline to spread the word, most people with apnoea don't realise they have information technology.
A 2022 German written report found that while obstructive sleep apnoea might be nowadays in as much as twoscore% of the general High german population, but i.8% of hospital in-patients were identified as having it, which the authors said was perhaps due to low awareness of the condition amid both patients and hospital staff.
Co-ordinate to an article in the New England Journal of Medicine, there's an "epidemic" of sleep apnoea amongst US surgical patients. 1 in iv candidates for elective surgery take information technology, but for certain groups, the rate is fifty-fifty college – 8 in ten patients being treated for obesity, for instance, have information technology, resulting in a range of risks.
"Patients with sleep apnea undergoing orthopedic or full general surgery appeared to be at increased adventure for pulmonary complications and demand for intensive care services, which significantly increase health care costs," the authors noted.
My revealing on the pre-surgical questionnaire that I previously was diagnosed with sleep apnoea had immediate furnishings. My spine surgery was done quickly – taking place a week after I outset went over my MRI with a surgeon – merely in that brief period the hospital insisted I undergo a home slumber written report to approximate the severity of the apnoea. Instead of going to a sleep centre, I brought abode a kit that instructed me how to place sensor bands around my chest, a pulse oximeter on my finger, and a clip under my nose to monitor animate. In that location was no EEG, and one drawback of these take-home tests is the units never know if you are actually comatose or not while the readings are existence fabricated.
Nonetheless, lowering the cost and inconvenience of diagnosis offers hope that more people will discover they accept apnoea – the expense and time needed to have an in-lab polysomnogram is thought to exist one reason diagnosis rates are so low.
The examination found I had moderate apnoea – possibly a function of keeping that terminal 10 pounds off – data the anaesthesiologist used when putting me under.

A dental appliance that brings the lower jaw forward has been used to care for sleep apnoea since the 1990s (Credit: Getty Images)
"Weight loss is curative," says Philip Smith, a professor of medicine at Johns Hopkins School of Medicine and a specialist in pulmonary illness and slumber apnoea. "The problem is, people can't do it."
Add to this the fact that many patients can't use CPAP, and it becomes articulate that in that location'southward a "critical unmet need," says Schwartz. Then over the past two decades, a series of other treatments take been rolled out.
In the mid-1990s, a dental appliance began to be used by those who couldn't tolerate the mask.
"Obstructive sleep apnoea happens in the dorsum of your mouth," says David Turok, a general dentist with a practice concentrating on apnoea. "Basically, your tongue doesn't have enough room in your mouth and pushes back into your airway. CPAP forces the natural language out of the way by forcing air down. An oral appliance brings the lower jaw forrad, and the tongue comes with it."
Think of it as a brace, using upper teeth as an ballast to push button the lower teeth, and with them the lower jaw, forward, widening the airway at the back of the throat.
Like CPAP, the oral appliance is besides an imperfect solution. It holds the jaw in an unnatural position, and so information technology tin can be uncomfortable, and prolonged use tin change your bite, leaving the jaw forward. The force per unit area of information technology tin can also change the position of your teeth a lilliputian bit.
Yet in his years of working on apnoea treatments, the majority of Turok'southward patients have had success with an oral appliance.
"Merely these are mild-to-moderate cases," he says. "For someone with severe sleep apnoea, CPAP is preferred. I never say you have a choice. You've got to try CPAP first."
He says that the surest style to address apnoea, for patients who can't suit to either CPAP or oral appliances, is jaw-advocacy surgery, a better procedure than widening the soft tissue of the throat.
"Recovery is easier because it is os healing instead of tissue healing," Turok says. Though the surgery is not without drawbacks, including the need to pause your lower jaw in two places and accept your mouth wired shut after surgery.
A further strategy is, in essence, an electrical version of the oral appliance: hypoglossal nerve stimulation (HNS), where a small electrical accuse is used to make the tongue contract and stop it falling backwards during sleep.
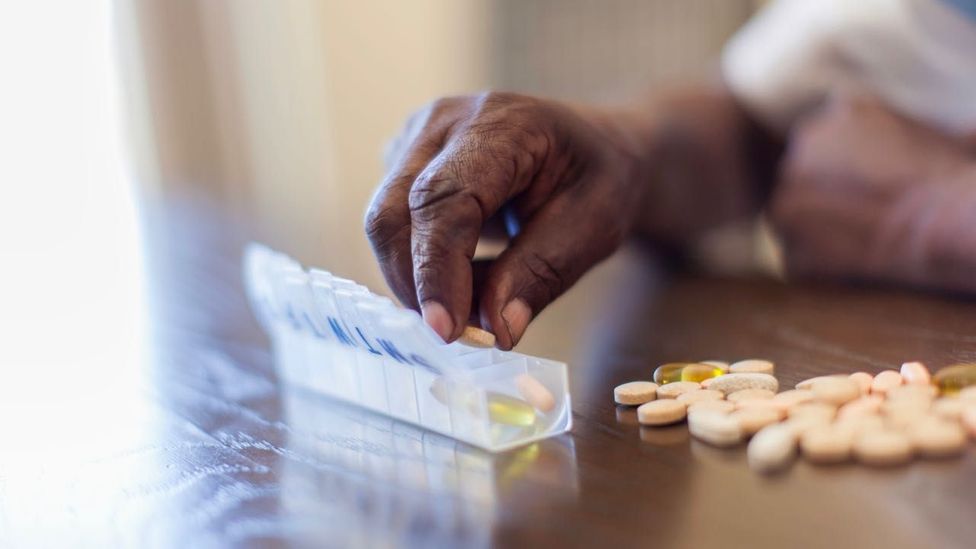
Researchers hope to have a pill to treat sleep apnoea in the next decade. (Credit: Getty Images)
Lawrence Epstein, banana medical managing director of the Sleep Disorders Service at Brigham and Women'south Hospital in Boston and past president of the American Academy of Slumber Medicine, calls CPAP "the recommended first-line therapy," but says handling ultimately is "more about knowing all the options and trying to tailor the therapy both to what the patient has and what they would be willing to use".
He points out that while obstructive slumber apnoea is viewed as a single condition, it is prompted by a multitude of causes – facial and throat configuration, muscle tension, obesity – and and so non every handling works the aforementioned for every patient.
"We have very effective treatments, but all have some downsides. It's a thing of matching the right treatment to the right patient."
There really is but 1 test: "Make sure it works," he says, noting that "we still accept a ways to go" when it comes to perfecting handling.
Much hope is centring on that treatment someday being a pill.
"The time to come is neurochemical," says Smith of Johns Hopkins. "We tin care for apnoea in a mouse. Probably in the side by side ten years, perhaps five, yous'll be able to take medication for slumber apnoea, because information technology's a neural-chemic problem. It'due south not obesity itself, not fat pressing on the airway, but fat excreting certain hormones that makes the airway collapse." Schwartz is more than attentive – he thinks "it'due south a combination of the two" – but has as well been investigating hormones secreted by fat cells.
At that place are too promising human being trials. Phyllis Zee was co-pb writer of a 2022 newspaper that plant that dronabinol, a synthetic version of a molecule found in cannabis, is "safe and well tolerated" and lowers the severity of sleep apnoea compared to a placebo.
"The CPAP device targets the concrete problem but non the cause," Zee said at the time of publication. "The drug targets the encephalon and fretfulness that regulate the upper airway muscles. Information technology alters the neurotransmitters from the brain that communicate with the muscles."
At that place are other hopeful signs. A small double-blind international study of 2 drugs used in combination – atomoxetine and oxybutynin – found that they "profoundly reduced" apnoea, cutting airway obstructions during sleep past at to the lowest degree 50 per cent in all of the participants.
But for a person like me, struggling with apnoea now, the expect might exist a long i.
"They've been predicting in 20 years we're going to have some drug to deal with the problem," says Schwartz. "The only trouble is, it's been a rolling twenty-year excess. We'll get at that place, I accept no doubt. There are a couple of promising pharmacological approaches that may be on the horizon."
Patience and healthcare are ofttimes linked, whether waiting for new treatments creeping to marketplace, waiting for changes in lifestyle to conduct fruit, or even waiting to run across the right specialist. For me, it was back to long-term dieting and an appointment with a sleep specialist at Northwestern.
Every bit an indicator of just how many people are dealing with this status, I got in bear upon with Northwestern in July, when I had my surgery and learned the apnoea had returned. They said they would schedule me for the showtime available appointment – not until late Oct.
This is an edited version of an commodity that first appeared on Mosaic and is republished here under a Creative Eatables licence.
--
Join 1 million Future fans by liking united states on Facebook, or follow us on Twitter or Instagram.
If y'all liked this story, sign up for the weekly bbc.com features newsletter, called "The Essential Listing". A handpicked selection of stories from BBC Futurity, Culture, Worklife, and Travel, delivered to your inbox every Friday.
Source: https://www.bbc.com/future/article/20200305-sleep-apnoea-the-people-who-stop-breathing-in-their-sleep
Post a Comment for "My Cpap Gave Me Life Again I Lost Weight I Wasnt Depressed"